Is Clinical Practice a Science or an Art?
As a non-medic, this is a question that I have asked numerous healthcare professionals over my career.
I have received many illuminating responses and the simplest one that I understood was that medicine is the application of experience to the specific (patient-centred) clinical situation being faced – an expert combination of subjectivity and objectivity. This responder also suggested that the reference points for clinical practice can (and should) change over time as more evidence, experience and opinion comes to the fore.
Other colleagues have asserted that one source of evidence doesn’t necessarily ‘trump’ the other – all available evidence should be considered, accepted, or dismissed collectively.
Evidence comes in different forms and incorporates the available body of information indicating whether a belief or proposition is true or valid. Healthcare is advancing quickly and there are new innovations creating some ambiguity in practice.
The increasing complexity of healthcare could be driving further ambiguity in the clinical environment today. The examples of this, whilst not exhaustive, include the introduction of Chimeric antigen receptor (CAR) T-cell therapy, and other more specialised/personalised treatments with less mature or incomplete data at launch, the role of combination therapy in a myriad of oncology settings, and understanding how to address new diseases such as Cov-SARS-2. Undoubtedly, some RCTs absolutely drive clinical practice such as the 4S study in cholesterol lowering (1994) and the UKPDS study in glycaemic therapies (1997), but not all studies are equal and the range available to clinicians is expansive:
- Randomised controlled trials (RCTs)
- High quality meta-analysis
- Systematic reviews of RCTs
- High quality systematic reviews
- Well conducted case control or cohort studies
- Non-analytical studies, e.g. case reports, case series
- Expert opinion
- Real-world data, audits and registries
- Retrospective studies
- Health economic data
- QoL studies
- Time in motion studies
What type of evidence is available?
Feeling intrigued, with further investigation, it is interesting to note what type and amount of published evidence was available to inform clinical practice.
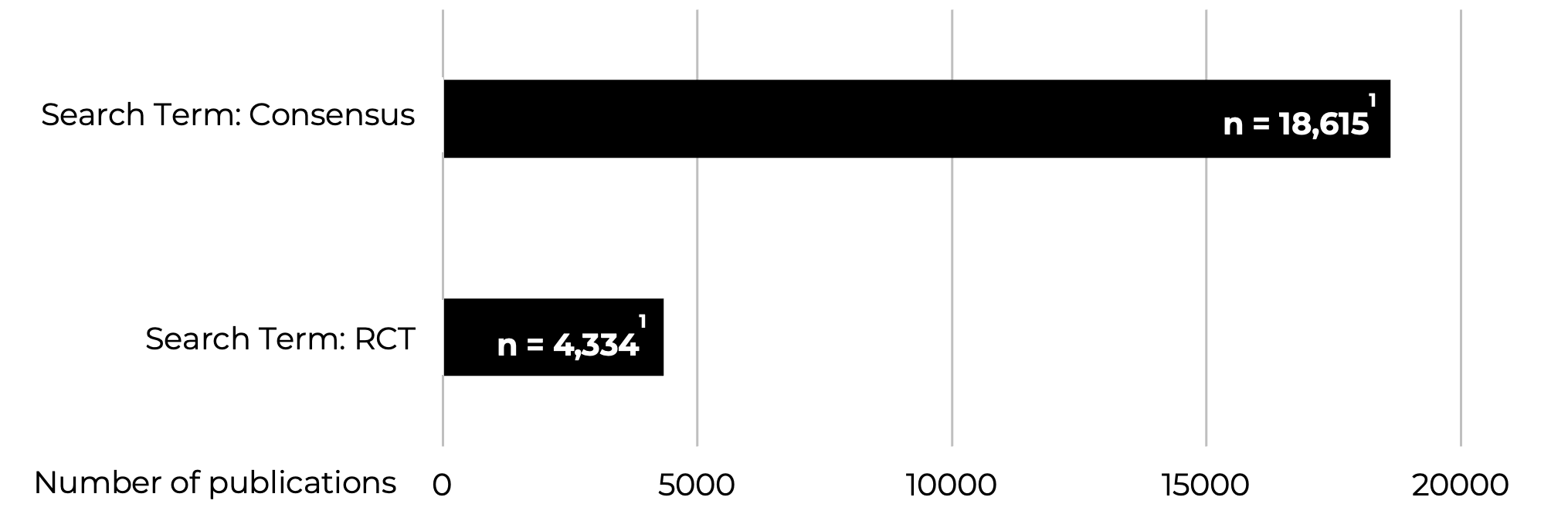
A simple PubMed search (using MeSH terms) demonstrated the number of published RCT studies versus opinion/consensus studies in 2021.1. It showed that more opinion-based evidence, such as delphi consensus-derived evidence, was published in 2021 compared to RCTs. Driven in part by the need to address answers to clinical questions to treatment and management of an emerging condition – Covid-19 but spanning a range of conditions and settings.
As recently as 2018, the primacy of randomized trials has been reconsidered because of the weaknesses of RCTs.2 How should opinion in clinical situations be best planned for, obtained and trusted?
It has been cited that stringent application of scientific research techniques, such as the expert Delphi methodology, allows survey of experts in a high quality and scientific manner.
Delphi is a robust, powerful and applicable medical communications approach, suited to a range of healthcare business situations. Any situation requiring better understanding, better decisions, better relationships and better implementation must be assessed so that the feasibility for Delphi communications can be expertly explored.
Consensus, without compromise
With its structured method of developing consensus among panel members, the Delphi consensus has gained acceptance in diverse fields of medicine, healthcare, and policy.
The Delphi method in healthcare assumed a pivotal role in the last few decades to develop best practice guidance using collective intelligence where research is limited, ethically/logistically difficult or evidence is conflicting. However, the attempts to assess the quality standard of Delphi studies have reported significant variance, and details of the process followed are usually unclear.
Triducive recommend systematic quality steps for evaluation of Delphi methodology; identification of problem area of research, selection of panel, anonymity of panellists, controlled feedback, iterative Delphi rounds, consensus criteria, analysis of consensus, closing criteria, and stability of the results.
Variants have been developed from the basic technique and applied across healthcare, now being applied with more heterogeneous expert groups working across healthcare.
The opinion of experts counts
Delphi communication was originally introduced and practiced dealing with technical topics and to seek consensus among homogeneous groups of experts. The RAND Corporation is usually acknowledged as having conducted the earliest Delphi studies in the 1950-60s.4
The types of opportunities for this approach in healthcare are:
- Establishing a focus on unmet clinical needs
- Stimulating and supporting optimal healthcare practice
- Supporting new/updated healthcare policy
- Defining patient cohorts
- Identifying risk factors of disease
- Identifying barriers to access of services
- Developing pathways
- Understanding future research needs
- Developing expert guidelines
- Understanding and mobilising medical advocacy
- Establishing new practice
- Exploring practical applications to evidence-based medicine
Often with healthcare and pharmaceuticals, we find that the product attributes and profile is pre-established and substantiated; the health economics is balanced for favour. As competitive healthcare business professionals, there is limited latitude as to what we can do with the product or price, especially with an established cohort of clinical customers. Differentiating the brand proposition (i.e., features versus gains and benefits) is one way to address value gaps, but most of this has been pre-defined, often by the clinical trial programme and health economic modelling.
Clinical practice evolves for many reasons, but also by deliberate design and through market shaping initiatives. Others (e.g., patients, key opinion leaders, competitors, customers, policy makers, budget holders, media) all have a role to play in effective and efficient clinical practice – they may contribute to future practice and healthcare product development.
- Any evolution in clinical practice demands:
- A deeper understanding
- To reach better decisions
- That results in better implementation
- Through fostering better relationships
Clinical practice appears to be informed by a range of evidence. It still seems a combination of science and art. With even more ways to find the answer to complicated and demanding clinical questions, finding the right evidence is important. As supported by research bodies, expert opinion remains a necessary component in the armamentarium used to determine the answer to a clinical question.
Globally, Triducive work with clinical experts, policy makers, industry, academia, patient groups and the third sector to get better decisions made and implemented.
They all benefit from the scientific Delphi approach through:
- A real-world perspective (which often lacks in methods ranked higher in the hierarchy of evidence);
- A decision-making process attempts to generate as much agreement as possible;
- Actively soliciting the input and participation of all decision-makers;
- Participants striving to reach the best possible decision for the group and all of its members, rather than competing for personal preferences;
- Participants shaping a decision that meets the concerns of all group members as much as possible;
- As many stakeholders as required involved in the decision-making process;
- All members being afforded, as much as possible, equal input into the process.